
Often, women have a negative attitude toward sex. And this is not the fault of education or moral principles but an elementary fear of conception. In the age of the latest medical technology, abortion is not painful but emotional experiences are immense.
Not many women will dare to give birth to one child after another, and often they have to terminate a pregnancy against their will. Afraid of getting pregnant, the young woman is looking for excuses to avoid the embrace of her husband, and the harmony of family life begins to crumble.
All of this can be avoided if affordable contraceptives are used correctly. In this article, we will review the recommended and affordable contraception options for women in their 20s.
Reasonably priced birth control options for 20- to 29-year-old women
Pills
Oral contraceptives are theoretically more than 99% effective.
The most common method of use is that oral contraceptives are taken at the same time every day for 21 days, followed by a seven-day break during menstruation; or taken at the same time every day for 28 days, without any breaks (in this case, the pack contains 7 placebo pills that serve as reminders. Most drugs contain estrogen ethinylestradiol at a dosage of 20 mcg and one of the gestagen types:
- norethindrone;
- levonorgestrel;
- norgestrel;
- norgestimat;
- desogestrel;
- drospirenone.
A new trend in the production of oral contraceptives is the release of drugs that increase the level of folate in the blood. These pills contain drospirenone, ethinylestradiol and calcium levomefolate (a metabolite of folic acid) and are indicated for women planning a pregnancy soon.
Monophasic birth control pills s have a constant dose of estrogen and progestin. Two-phase pills contain two different doses of estrogen and progestin, three-phase – three, and four-phase – four combinations of estrogen and gestagen. Multi-phase drugs do not have advantages over monophasic combined oral contraceptives in terms of effectiveness and side effects.
The overwhelming majority of combination oral contraceptives available on the pharmaceutical market are monophasic.
Birth control pills work by inhibiting ovulation. The drugs reduce the synthesis of FSH and LH. The combination of estrogen and progestin has a synergistic effect, antigonadotropic and antiovulatory properties. In addition, oral contraceptives change the consistency of cervical mucus, cause endometrial hypoplasia, and reduce the contractility of the uterine tubes.
Their effectiveness is highly dependent on compliance. The frequency of pregnancy during the year ranges from 0.1% with correct use to 5% in case of violations in the usage.
Pros:
- Combined hormonal contraceptives are widely used to treat menstrual irregularities, reduce or eliminate ovulatory syndrome. These drugs reduce blood loss, so they are often prescribed to treat menorrhagia. They can be used to correct the menstrual cycle – if necessary, to delay the onset of the next menstruation;
- The pills reduce the risk of benign breast formations, inflammatory diseases of the pelvic organs, and functional cysts;
- They reduce the risk of malignant ovarian diseases by 40%, endometrial adenocarcinoma – by 50%. The protective effect lasts up to 15 years after the drug is canceled.
Cons:
- Birth control pills can cause side effects: nausea, breast tenderness, breakthrough bleeding, amenorrhea, headache;
- Estrogen, which is part of the drug, is able to activate the blood coagulation mechanism, which can lead to thromboembolism;
- The risk group for developing such complications while taking oral contraceptives includes women with high LDL cholesterol and low HDL cholesterol levels, severe diabetes accompanied by arterial damage, uncontrolled arterial hypertension, and obesity. In addition, women who smoke are more likely to develop blood clotting disorders.
Vaginal suppository
Vaginal suppositories are used locally – intravaginally. Spermicides destroy the protective membrane of the sperm. They separate the flagella from the heads and further completely destroy them.
It should also be noted that this medication is capable of providing antiseptic and antimicrobial effects. The active substance of suppositories is active against chlamydia, gonococcus, trichomonads, corynebacteria, herpes viruses, enterococci, staphylococci, cytomegalovirus, hepatitis B viruses, fungi of the genus Candida and HIV.
Suppositories act on the thickening of cervical mucus, resulting in a film that does not allow sperm to penetrate through the external os of the cervix.
Experts say that this remedy is not absorbed intravaginally. Moreover, it is absorbed only by the walls of the vagina.
The drug is removed from the body along with physiological secretions. It can also be removed by douching with plain water.
The vaginal suppository is used as local contraception when:
- IUD or oral pills are contraindicated;
- The woman is breastfeeding or has recently given birth to a child;
- A woman had an abortion or miscarriage;
- Sex life is irregular;
- The woman is premenopausal;
- The woman wants to take a break from using oral pills (suppositories can be combined with other contraceptive drugs).

Encare Review
- Active Ingredient: Nonoxynol-9
- Release Form: Vaginal Suppository
- Age: 18 - 55 years
- Average Price: $200 - $220
Vaginal ring
The contraceptive vaginal ring is hormonal birth control. The effect is provided by ethinyl estradiol and segesterone; or ethinyl estradiol and ethonogestrel.
The structure of the contraceptive ring is simple. It is a silicone translucent rim, easily reshaped. The diameter of the protector is 5-6 cm.
Every day, a certain dose of active substances is released from the hormonal ring. They are absorbed into the vascular network of the vagina and enter the bloodstream.
The action of the drug begins immediately after insertion and ends after withdrawal. Using a vaginal ring has the following effect:
- prevents the growth of follicles, their opening and the release of the egg;
- disrupts the process of endometrial proliferation, which creates unfavorable conditions for implantation;
- organizes a special hormonal background, which allows not only to protect against pregnancy but also to get a therapeutic effect;
- affects the secretory activity of the cervix, as a result of which the mucus thickens and reduces the activity of the spermatozoa that have entered it.
The action of the ring is a reversible process.
The vaginal ring makes periods regular, less heavy, and less painful. It also reduces the risk of iron deficiency anemia.
The main advantage of the hormone-based contraceptive ring is that its use prevents:
- ovarian cancer;
- endometrial cancer;
- ovarian cysts;
- ectopic pregnancy;
- inflammatory diseases of the genital organs;
- benign neoplasms in the mammary glands.
Pros and cons of using the contraceptive ring:
- It helps prevent unwanted pregnancy without the additional use of barrier methods of contraception and pills;
- The device has many contraindications and sometimes causes side reactions;
- Before use, you must carefully study the instructions, and it is better to consult a specialist.
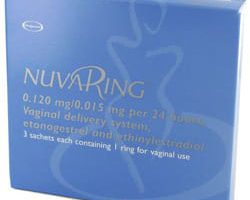
NuvaRing Review
- Active Ingredient: Ethinylestradiol / Etonogestrel
- Release Form: Vaginal Ring
- Age: 18 - 40 years
- Average Price: $165
Injection
Hormonal injections are a method of hormonal contraception that involves the administration of hormonal contraceptives by injection. Women are given intramuscular progestin injections every 3 months. This method if not very popular since the injection of a progestin, like any other injection, is very painful. Hormonal contraceptives can just as well be absorbed in the intestines, and this procedure is completely painless, unlike hormonal injections. Therefore, women prefer oral contraceptives to hormonal injections, but hormonal injections usually have one advantage: one injection is enough to maintain the contraceptive effect for several months. Contraceptive drugs for men are still quite ineffective and have many side effects, but injections are still the only method of introducing them into a man’s body.
Mechanism of action:
- suppresses ovulation;
- changes the structure of the endometrium (the lining of the uterus) – the fertilized egg cannot attach to the walls of the uterus;
- thickens cervical mucus, making the cervix impassable for spermatozoa;
- affects the motor ability of sperm, making them less mobile.
The contraceptive injection does not protect against STIs or HIV. Only a condom can provide this protection.
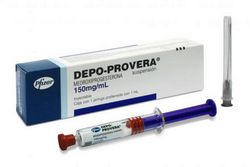
Depo-Provera Review
- Active Ingredient: Medroxyprogesterone Acetate
- Release Form: Suspension for Injection
- Age: 18 - 45 years
- Average Price: $110
Depo-Subq Provera 104 Review
- Active Ingredient: Medroxyprogesterone Acetate
- Release Form: Suspension for Injection
- Age: 18 - 45 years
- Average Price: $250
Transdermal patch
A contraceptive patch is like a regular, smooth patch applied to your skin. It is highly effective in preventing pregnancy. The hormones estrogen and progestin continuously pass through the skin into the bloodstream, blocking ovulation and also thickening cervical mucus that prevents sperm from entering the egg. The patch is not transparent, so this method of contraception is visible.
The hormones only last seven days. Therefore, the patch must be changed weekly. Regularity is important in using the patch.
A contraceptive patch can save 98% from unwanted pregnancy if used correctly, but in case of violations, the indicator decreases to 91%.
Pros:
- high efficiency (91%);
- easy to use;
- does not require daily attention;
- makes spontaneous sex possible and does not affect the sensations of intercourse.
Cons:
- visible on the skin, may fall off;
- requires schedule monitoring;
- may cause slight itching and redness at the site of application;
- may cause migraines, weight gain, and mood swings in some women;
- may cause irregular periods;
- in rare cases, some women may have the risk of blood clots, heart attacks and strokes;
- does not protect against sexually transmitted diseases.
This type of contraception is not suitable for smokers or women with high blood pressure.
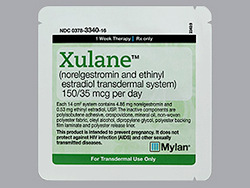
Xulane Review
- Active Ingredient: Ethinyl Estradiol / Norelgestromin
- Release Form: Transdermal Patch
- Age: 18 - 45 years
- Average Price: $120
Lo Loestrin Fe Review
Layolis Fe Review
Jolessa Review
Introvale Review
Drospirenone / Ethinyl Estradiol / Levomefolate Calcium Review
Rajani Review
Ocella Review
Seasonale Review
Tydemy Review
Safyral Review
Natazia Review
Balcoltra Review
Ashlyna Review
Dienogest / Estradiol Review
Slynd Review
Drospirenone Review
Norinyl 1+50 Review
LoSeasonique Review
Daysee Review
Amethia Review
Seasonique Review
Camrese Review
Rivelsa Review
Fayosim Review
Quartette Review